The Ultimate Gut Protocol: SIBO, Leaky Gut, and Everything In Between
How I fixed my gut from Crohn's, C. diff, SIBO, Blood Clots, and more
Over the past couple of years in the alternative health space, gut health has largely taken the spotlight. Most people have dealt with gut issues in some form or fashion: indigestion, bloating, gas, burping, etc.
I’ve heard from clients, friends, family, and folk off the street about parasite cleanses, probiotics, and raw milk.
Coming from someone who is missing his colon from Crohn’s disease, has battled deadly gut bacterial infections on multiple occasions (Cdiff), and done loads of antibiotics, I feel fairly qualified to speak on gut health.
This is why I am especially excited to write this post. A healthy gut is an essential step in achieving optimal health.
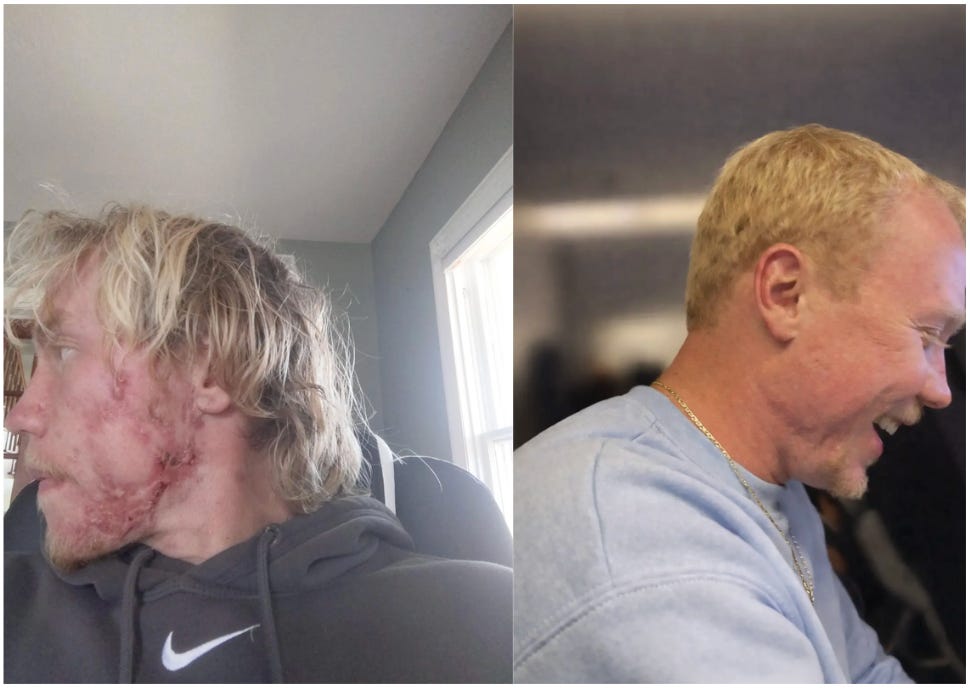
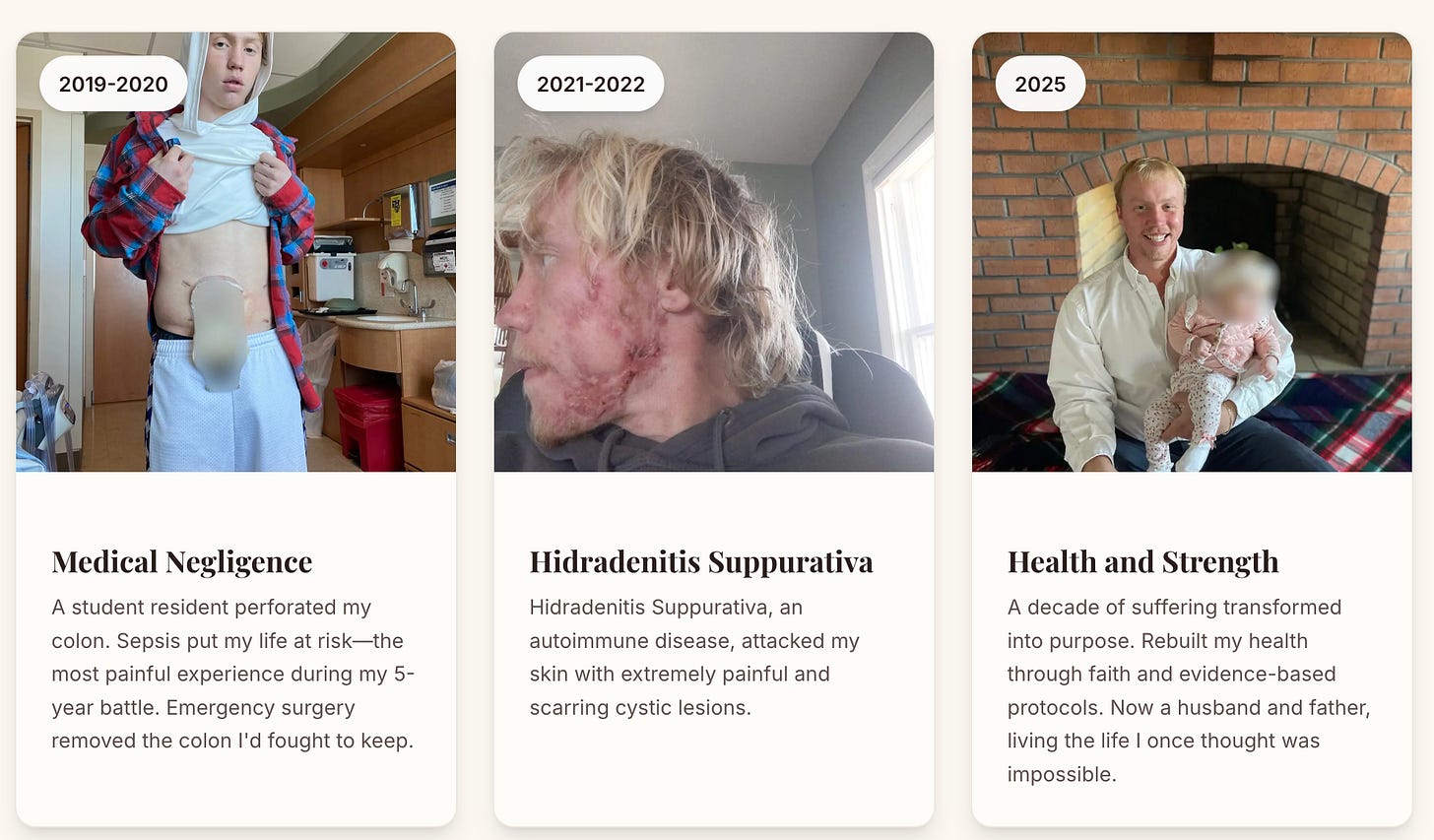
Before I fully addressed my gut health and other root cause issues, then After!
SIBO
The management of Small intestinal bacterial overgrowth (SIBO) is crucial for gut health. SIBO is one of the most common issues associated with poor gut health, and controlling and eradicating it is key to a healthy gut.
Take IBS, for example, which allopathic medicine has lazily mistaken for SIBO. Irritable Bowel Syndrome essentially means they don’t know what it is or how to fix it; a rather ambiguous diagnosis that provides zero helpful information, yet is thrown at anyone with gut discomfort.
If someone tells me they have IBS, I reframe that to “Oh, you have SIBO, you mean?” IBS and SIBO share the same symptoms.
Symptoms like: Excessive burping after eating, bloated stomach in the morning, overly gassy, indigestion, poor nutrient absorption, irregular bowel movements, brain Fog, excessive fatigue post-meal.
In reality, most Americans would likely check the box for almost all of these symptoms, even among the most health-conscious people.
Whether it’s disguised as an IBS label or not, SIBO is prevalent in a vast majority of the population.
SIBO occurs when an overgrowth of microbes, typically belonging to the large intestine (colon), colonize in the small intestine.
This can happen in several ways: harmful bacteria surviving the stomach’s acid and poor bile function , slow gut motility, antibiotics , glyphosate, heavy metals, and poor immune function (gut contains 80% of the immune system).
The primary function of the small intestine is to break down food and absorb nutrients. For this reason, it has a single mucosal layer, rather than the colon’s double layer, which naturally makes it more permeable, but less robust to bacterial infiltration.
SIBO erodes this mucosal layer, leaving the gut lining susceptible to food particles, dead bacterial cell components (LPS/endotoxins), and toxins, all of which leak into the body through the exposed gut wall.
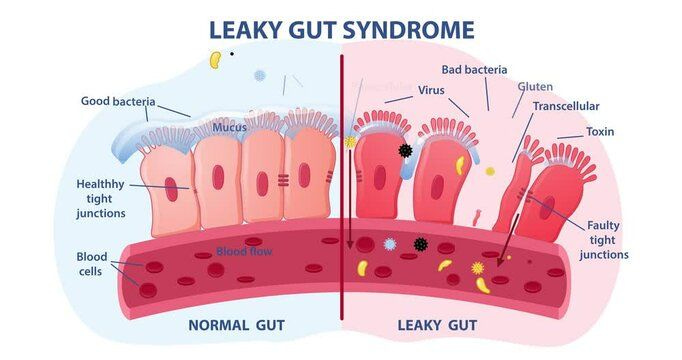
This is essentially leaky gut. When the mucosal layer of the gut is broken down, leaving the epithelial cells and tight junctions binding them together vulnerable, which are later damaged, creating “leakage” into the tissue and vasculature.
LPS
LPS (lipopolysaccharide/endotoxin) is a toxic molecule that forms part of the outer wall of gram-negative bacteria, such as E. coli and Salmonella. These gram-negative bacteria are amongst the most common in SIBO infections. These bacteria are so toxic that 1-2mg of LPS injected intravenously can be lethal!
Picture this: you develop SIBO after something like antibiotics, heavy metal exposure, or having poor stomach acid. Your mucosal layer breaks down due to the overgrowth of bacteria, and your epithelial cells and tight junctions are damaged.
Right beneath the epithelial cells sits the gut-associated lymphoid tissue (GALT). The GALT layer makes up roughly 70% of your body’s immune system. The GALT layer is programmed and well-suited for interactions with LPS. When LPS is detected, an immediate and aggressive response is triggered.
The immune cells launch a rapid inflammatory cytokine storm, attempting to neutralize the LPS molecules.
Normally, the body is well prepared for LPS leakage and has layers of tissues that prevent large amounts of LPS from entering the bloodstream.
Yet, with SIBO, this becomes a continual fight. The SIBO bacteria are constantly eroding the small intestine’s protective layers, dying off, and leaking LPS into gut tissues. Chronic inflammation begins to develop as the immune system is perpetually under pressure.
The Downstream Effects
With almost 5% of Americans being diagnosed with autoimmune diseases, they have become rampant amongst the general public here in the West. Could endotoxemia be a major trigger for the irregular immune function involved in autoimmune?
A 2022 study found associations between autoimmune, digestive disorders, heart issues, blood clotting, and more with SIBO.
Some of those included:
Gut & Digestive Irritable bowel syndrome (IBS), Crohn’s disease, Ulcerative colitis, Celiac disease, Non-alcoholic fatty liver disease (NAFLD), Cirrhosis, Chronic pancreatitis, Gallstone disease
Heart & Circulation Heart failure, Atherosclerosis, Deep vein thrombosis
Hormonal & Metabolic Type 1 and Type 2 Diabetes, Hypothyroidism, Hyperthyroidism (Graves’ and Hashimoto’s)
Brain & Nervous System Parkinson’s disease, Brain fog, Autism spectrum disorder
Immune & Autoimmune Systemic sclerosis, Rosacea, Chronic kidney disease
So why would SIBO be linked to autoimmune, and where does LPS fit into this picture? It’s called molecular mimicry. It is where Gram-negative bacteria closely resemble the molecular structure of your own cells.
When the GALT layer raises its attack against LPS, antibodies are produced.
Eventually, under the constant burden of SIBO, those antibodies start confusing the LPS structure with the body’s structure. What serves as a protective mechanism for the bacteria leads to the immune system malfunctioning, causing it to confuse friend from foe.
It’s almost like D-Day for your immune system; the sheer overwhelm causes it to fire on anything that moves.
Personally, this theory has resonated with me, given my history of Crohn’s, two deep vein thrombosis blood clots, Hidradenitis suppurativa, and several intense bouts with CDiff infections.
A common thread to SIBO and when I was first diagnosed with Crohn’s was that horrific C. diff infection. CDiff creates terrible gut dysbiosis (more harmful bacteria & less microbial diversity) and SIBO, inviting in all the bad guys like Clostridium perfringens, Staphylococcus aureus, Klebsiella oxytoca, Candida spp., and Salmonella spp.
Basically, one bad dude gets in there, beats up the good guys, destroys the gut lining, and invites all the other opportunistic bad guys. You couldn’t ask for better conditions if you were a SIBO bacterium.
What’s even more intriguing is that a fecal microbiome transplant, for my CDiff infection, is what put me into remission for several years; it was almost instantaneous as well.
It was like reseeding my lawn. My overgrown, messy, weed-filled lawn was aerated and reseeded with a healthy new seed. The new seed started crowding out the weeds, almost like a yin-yang relationship.
If you’re tired of guessing and want help getting to the root cause of your issue, try my Root Cause AI found on my website: littlewaycoach.com. It pairs great with the root cause quiz!
Another anecdote of mine that surprised me was that Deep Vein Thrombosis (DVT) has been linked to SIBO. Looking back now it makes sense, but whenever I would have a bad Crohns flare up, I would get a DVT. To no ones surprise, the allopathic doctors NEVER had an answer as to the root cause.
Well, turns out, LPS has been shown to interfere with an anticoagulant pathway in the body, specifically, the protein C anticoagulant.
Given my chronic Cdiff infections, it would make a lot of sense that immune dysfunction, caused by large LPS burdens, confused my immune system, creating an autoimmune disease and blood clotting.
Considering the amount of research on these connections, it wouldn’t surprise me. It was most certainly a major factor, amongst other things like blue light, mold, heavy metals, which, oddly enough, create a flywheel with SIBO and gut dysfunction, but that’s for another day ;).
Studies: Study 1, Study 2, Study 3, Study 4
Head over to littlewaycoach.com to take my root cause quiz, connected to a custom AI chatbot that gives you real answers about what’s going on with your health. Ask about SIBO!
What to do about it?
My philosophy around SIBO has come from a lot of trial and error on myself and others plus countless hours of research from some of the top experts.
One of those experts is Dr. William Davis, the author of Super Gut. Dr Davis describes how to combat SIBO utilizing a 36-hour fermented yoghurt made with three key microbes.
This strategy has worked really well for almost everyone I have recommended it to. While it can take a few tries to get the recipe and process down, it is well worth it.
Essentially, Dr. Davis found three key microbes that produce potent bacteriocins: peptides made by bacteria that have an antibiotic-like effect on other bacterial species.
Bacteriocins inhibit the growth or kill other bacteria, usually those of the same or closely related species. Bacteriocins from good bacteria like L. reuteri, L. gasseri, and B. subtilis, which are used in the SIBO yoghurt, target Gram-negative bacteria like E. coli and Salmonella.
For example, L. reuteri has been shown to “convert glycerol into a potent broad-spectrum antimicrobial compound, reuterin, which inhibits the growth of gram-positive and gram-negative bacteria.”
It’s an intelligent way to target harmful bacteria without harming the good guys.
Compared to other bacteria, these bacterial strains favor the small intestine, directly attacking the heart of the problem; an overgrowth of bacteria in the small intestine.
The reason it is better to consume the yogurt made by these piobiotics versus just consuming the probiotics themselves is upon fermenting them, they go from hundreds of billions to reaching around a trillion CFU per serving (half a cup); roughly a 1,000-fold increase!
These strains also exhibit unique characteristics to survive the stomach acid and bile, especially with the high counts coming from the 36-hour fermentation process.
It is still up for debate whether they take residence full-time in the gut; regardless, they still exert their function whether full-time or part-time!
This yogurt has been the cornerstone of any SIBO protocol I recommend, simply because it works so well. Usually, people see results in 4-6 weeks with daily consumption.
Find the L Gasseri and B Subtilis on my Fullscript store, linked directly to the products!
Anecdotal evidence has shown a more diverse microbiome post consumption of this yoghurt, as these strains bring in fellow good guys, not unlike how something like Cdiff brings in more bad guys.
While this yogurt sits at the top of the chain, I utilize some other incredible strategies as well. This next section will be an overview of these strategies.
Studies: Study 1, Study 2, Study 3, Study 4
Herbal killers
Herbs like oregano, thyme, artemisinin, clove, lemon balm, and garlic are all powerful natural means of destroying SIBO bacteria, viruses, and parasites! In fact, herbal antibiotic therapy is just as effective as antibiotics like rifiaxmin, which is commonly used for SIBO to inhibit the growth of bacteria in the small intestine.
Many of these plant compounds have been studied for treating infections, gut issues, or taking advantage of their antioxidant, antimicrobial, and anti-inflammatory properties.
For example, artemisinin has been known for its management of malaria since the 1970s, while it has recently been proposed as a covid therapy. It is also non-toxic and exerts a suppression of pro‑inflammatory mediators.
Personally, I am a big fan of herbal antibiotics for SIBO and have had great success with them.
Studies used for this section: Study 1, Study 2, Study 3, Study 4
My Favorite Product found on my Fullscript store for 25% off!:
Sunlight
Ideally, sunlight should be #1 in your health protocols — the benefits go way beyond the microbiome. I wrote a whole post on it. But specifically for SIBO, sunlight has a fascinating and under-appreciated effect on gut bacteria.
Hunter-gatherer tribes living near the equator, under year-round UV exposure, consistently show some of the most diverse and robust microbiomes ever studied. The Yanomami of the Amazon are a prime example: no sunscreen, no sun-protective clothing, yet their beneficial bacteria levels are unrecognizable compared to Westerners.
You might assume diet is the explanation. But when control groups were simply exposed to UV light, they began developing bacterial profiles resembling hunter-gatherers.
The Hazda tribe of Africa showed microbiome changes that tracked directly with the seasons — rising and falling with UV availability throughout the year.
The sun isn’t just food for your skin. The data suggests it’s foundational to a healthy gut too.
Studies used for this section: Study 1, Study 2
Fermented Foods
Foods like kefir, saurkraut, kimchi, and kombucha are all solid options for building a diverse microbiome. These foods contain beneficial microbes in high counts, which survive stomach acid, can help reduce inflammation, and even work against harmful bacteria like H. pylori.
A study looking at Kefir and its health benefits found that “kefir may work against obesity, diabetes, liver disease, cardiovascular disorders, immunity, and neurological disorders. Peptides, bioactive compounds, and strains occurring in kefir can modulate gut microbiota composition, low-grade inflammation, and intestinal permeability, which consequently may generate health benefits.”
Overall, kefir will bring in supportive microbes into the gut, ones that compete with SIBO strains. My primary fermented food is kefir, which I prepare using kefir grains and raw milk, allowing it to ferment for 1-2 days.
Studies used for this section: Study 1, Study 2, Study 3, Study 4
Bile and Liver support
The gut should always be talked about in tandem with the liver. First off, SIBO can cause liver dysfunction in the form of fatty liver, probably from its antagonistic effect on bile.
Bile produced by the liver acts as a digestive aid, a detoxifier, and an antimicrobial fluid. With SIBO, the bacteria have enzymes that “deconjugate” bile acids, essentially reducing their ability to perform these functions.
With the bile being reduced, fat digestion is impaired, deficiencies in fat-soluble vitamins can occur, and antimicrobial activity is diminished.
My LabCorp account showed 10 years of high liver enzymes. Once I addressed bile flow and SIBO, my liver has never looked better. It is also fundamental for detoxifying from mold, heavy metals, glyphosate, and other environmental toxins.
A few of my favorite bile flow enhancers to use for gut health: Phosphatidylcholine, Swedish bitters, Taurine, Eating cholesterol-rich foods like egg yolks.
One of my hall of fame products, from QuickSilver Scientific, is called Liver Sauce, it’s a nutracutacal blend designed for maximizing bile flow. Bitters #9 is also similar for more everyday use!
Phosphatidylcholine (PC), my favorite supplement of all time, has also been shown to rebuild the mucosal layer in the gut, accounting for more than 90% of the phospholipids in mucus, and help Ulcerative colitis achieve remission (6G per day).
My Favorite Products for bile support found on my Fullscript store for 25% off, linked directly to the products!!
Studies used for this section: Study 1, Study 2, Study 3
Head over to littlewaycoach.com to take my root cause quiz, connected to a custom AI chatbot that gives you real answers about what’s going on with your health. Ask about SIBO!
Butyrate
Butyrate is a postbiotic made from good gut bacteria after fermenting resistant starches like cooked and cooled potatoes or rice. It is a short-chain fatty acid that provides 70% of the energy to your colonic cells, stimulates the mucosal layer, and accelerates the assembly of tight junctions in intestinal epithelial cells.
If you have ever had raw butter, you would notice the smell is a little off; that is actually butyrate, and it’s prevalent in butter, cream, cheese, and milk. You can also supplement it directly with sodium butyrate.
My Favorite Butyrate found on my Fullscript store for 25% off!
Studies used for this section: Study 1, Study 2
Zinc carnosine
Compared to other zinc supplements, zinc carnosine has a much more pronounced effect on the gut mucosal layer and wound healing in the gut & stomach lining (epithelial cell growth), eradicating H. pylori and healing stomach ulcers.
It is a powerful supplement for sealing a leaky gut and restoring tight junctions. In a study examining intestinal permeability after intense exercise, patients who underwent a 14-day zinc L-carnosine treatment showed a 71% reduction in intestinal permeability compared to the control group.
In the same vein, non-steroidal anti-inflammatory (NSAID) drugs are notoriously bad for the gut, so much so that indomethacin (a NSAID) induced a 3-fold increase in intestinal permeability in human controls but not in subjects taking zinc L-carnosine.
Overall, it’s a fantastic supplement for gut health, especially for building and protecting the gut lining against LPS leakage from SIBO.
Linked directly to my Favorite Zinc Carnosine through my Fullscript store for 25% off!
Studies used for this section: Study 1, Study 2, Study 3
Lactoferrin + Colostrum
Lactoferrin is a powerful molecule inherent in the body found in the saliva, tears, mother’s breast milk, and mucosal lining of the gut. It’s a strong antimicrobial and antiviral, biofilm disruptor, and it brings the innate and adaptive immune responses into equilibrium.
Lactoferrin supports the growth of beneficial bacteria like Bifidobacteria and Lactobacilli while inhibiting pathogens like E. coli, Salmonella, and Clostridium.
Moreover, lactoferrin protects epithelial cells from death caused by LPS, actively up-regulates the tight junction proteins that hold the gut lining together, and enhances overall gut barrier function, further preventing LPS from reaching the GALT layer and beyond.
Lactoferrin in Fullscript store for 25% off!
Studies used for this section: Study 1, Study 2, Study 3, Study 4
BPC-157
A peptide is a short chain of amino acids. BPC-157 (Body Protection Compound 157) is a peptide that is naturally derived from a protective protein found in human gastric juice.
It’s highly effective at healing the epithelial cells, bringing blood flow to damaged sites for enhanced healing, and sealing the tight junctions. I have an article on it here!
BPC in Fullscript store for 25% off!
Saccharomyces Boulardi
Saccharomyces boulardii is a probiotic yeast. It’s unique in that it is particularly resistant to stomach acid, bile salts, and antibiotics. It survives the digestive tract and is out of the GI system within 3 days.
It fights off harmful bacteria and fungi like C. diff and Candida and prevents their overgrowth, while exerting a protective effect over healthy microbes; for this reason, it’s also a powerful adjunct to antibiotic therapy.
Saccharomyces boulardii is also an effective means to prevent damage from LPS and the subsequent inflammation, while eradicating SIBO with an 80% sucess rate in cirrhosis of the liver patients, drastically reducing LPS from crossing the gut barrier.
It produces proteins that degrade toxins created by harmful bacteria that cause diarrhea. It also aids in the production of short-chain fatty acids like Butyrate. S Boulardi also increases the amount of immunoglobulins, essential for fighting off harmful invaders, while lowering inflammatory cytokines like IL-8, IL-6, IL-1β, TNF-α, and IFN-γ.
I am a huge fan of S Boulardi and rank it very high on the gut health list. If you have SIBO or some gut infection, SB should be close to #1 on your list. Personally, I make SB juice! I take one cap of SB probiotic and crack it into an organic juice. It’s a similar ROI to the yoghurt in terms of its huge return on overall count.
SB in Fullscript store for 25% off!
Studies used for this section: Study 1, Study 2, Study 3, Study 4, Study 5
Vitamin B1 Thiamin, TTFD version
Thiamine deficiency is increasingly recognized as a hidden driver of gut dysfunction. Thiamine supports energy production, nerve signaling, and gut motility, so low levels can contribute to bloating, constipation, nausea, reflux, and sluggish digestion.
Studies used for this section: Study 1
Activated Charcoal
Charcoal is a must for any gut protocol attempting to clear SIBO. Why? It binds to the LPS molecules as the SIBO bacteria begin to die off. This is what is referred to as “die off” and can cause herxeimer reactions from an increase in LPS as a result of killing the bacteria.
Of the mice given direct LPS injections, mimicking a sepsis occurrence, 13/13 mice given charcoal survived after 12 hours, compared to 0/13 not given charcoal.
Charcoal is one of the most effective means of binding LPS in the gut and preventing it from causing issues. When I first started addressing SIBO, I was not using charcoal and getting horrible die-off symptoms. When I added charcoal, I felt about 10x better. Always take ~2 hours away from medications and supplements!
Studies used for this section: Study 1
Conclusion
This stuff took me years of suffering, research, and personal experimentation to piece together. Crohn’s, C. diff, DVTs, hidradenitis — I’ve been through it, and gut health has been central to every single one of those battles.
This is why I offer health coaching: to help people who are suffering. If you’re tired of endless trial-and-error and want personalized guidance from someone who’s actually walked this path, book your free 20-minute consultation.
Let’s see if I can help you write your own transformation story.
Visit my website littlewaycoach.com! You can take a root cause quiz hooked into my custom AI chatbot for answers regrading your health concerns.
For anyone looking to get started on the supplement side, I put together a Fullscript plan with everything mentioned in this post — already curated, already dosed right, and you get 25% off through my link. No hunting around Amazon hoping you’re buying the right thing. It’s all there.
Till next time,
Scott
Disclaimer: This content is for informational purposes only and should not be considered medical advice. All opinions expressed are my own and not intended to replace professional medical guidance.










Three days after arriving home from a trip to Japan, my 18 yr old son started having severe abdominal pain. Over the next month, with four trips to the ER and no answers from the docs other than "accute inflammation in the small intestine" despite alllll the testing and antibiotics he was down 15 lbs, passing blood both ways and couldn't control the pain at all. Super scary. I was treating him myself with supplements like L Reuteri and mastic gum, but the game changer was BP 157. He had an endoscopy four days after his last trip to the. ER, after which I started him on the peptide, and it didn't show anything but healing areas. I'm not a doc, just a mom desperately trying anything to help my son, but that one turned my head for sure. The medical establishment was a near complete fail.
Thank you so much for this article